WISDOM TOOTH EXTRACTION/REMOVAL
WISDOM TOOTH EXTRACTION/REMOVAL
What are they
Wisdom tooth (your third molars) are the last teeth to come in – and the ones least needed for good oral health. They may not erupt or emerge from your gums until your late teens or early twenties – if they erupt at all. Most often, they’re impacted or trapped in the jawbone and gums, usually because there’s not enough room for them in your mouth. Our jaws are smaller than those of early humans who needed large jaws and more teeth for their tougher diet. We don’t need that extra chewing power anymore. In fact, wisdom teeth often do more harm than good.
From Silent to Serious Problems
If they’re impacted, you may not even know you have wisdom teeth – until pain suddenly strikes because of infection or pressure on an adjacent tooth. Partially erupting wisdom teeth may cause crowding or shifting of your teeth. You may not know that your developing wisdom teeth are pushing on the roots of adjacent teeth until those teeth start to shift. If your wisdom teeth do erupt, they may be hard to clean, so the odds of decay or infection of surrounding gum tissue are high.
Removal May be Wise
Whether you have obvious symptoms or not, you can rely on our expertise to diagnose existing or potential problems cause by your wisdom teeth. If our recommendation is their removal, it may be the wisest choice for the health of the rest of your mouth. Your wisdom teeth may be removed by us or we may recommend that you be attended to by an oral and maxillofacial surgeon (a mouth and jaw surgery specialist). You can help make your treatment a success by understanding why your wisdom teeth may need to be removed, what the procedure involves and what you can do to promote a successful recovery.
Understanding Your Wisdom Teeth
Most people have four wisdom teeth, one in each corner of the mouth, but each tooth can be at a different stage of eruption and position of impaction. Since wisdom teeth develop over a period of many years, harmful changes in your mouth may be gradual. But these changes could result in sudden and severe pain. If you learn the different ways wisdom teeth can develop, you’ll be better able to understand why you may need to have them removed.
How Your Wisdom Teeth Grow
By your late teens, your jawbone has nearly reached its adult size. But sometimes it isn’t big enough to hold developing wisdom teeth. When this happens, your teeth become trapped in the bone and grow wherever they can. The crown (chewing surface of the tooth) may only partially break through the gum. In other cases, it may remain completely in the bone. The roots, which hold the tooth in place, may become misshaped or grow dangerously close to a sinus cavity or to the nerve located in your lower jaw.
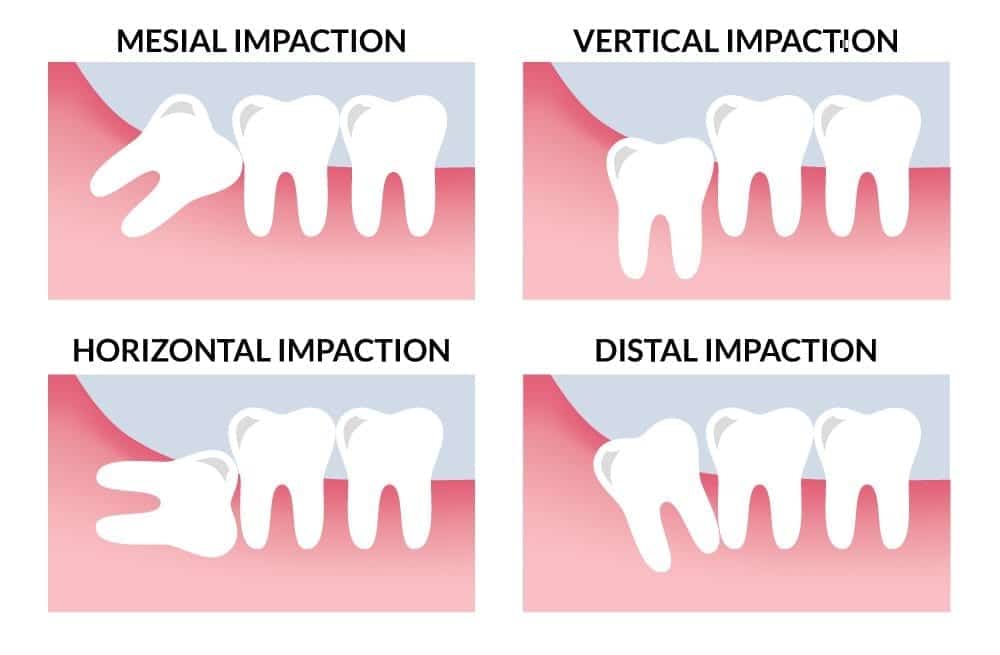
Positions of Impaction
Cramped for room, impacted wisdom teeth grow in many different directions, commonly at an angle. A wisdom tooth may grow at an angle toward your other teeth (mesioangular position) or away from your other teeth (distoangular position). They also can grow into a horizontal or vertical position.
The Advantages of Early Removal
Like all teeth, wisdom teeth develop inside an opening (socket) in your jaw, protected by bone and gum tissue until they erupt. Over time, your wisdom teeth become more firmly anchored in your jaw as their roots lengthen and the jawbone becomes more dense. So, the older you are, the more difficult it is to remove your wisdom teeth.
Wisdom Teeth Problems
Whether wisdom teeth cause your mouth harm depends on several factors, including the size of your jaw and how your wisdom teeth grow in. Sometimes, problem wisdom teeth cause symptoms like pain and swelling. Or you may have no symptoms at all but the other teeth in your mouth could be at risk for damage.
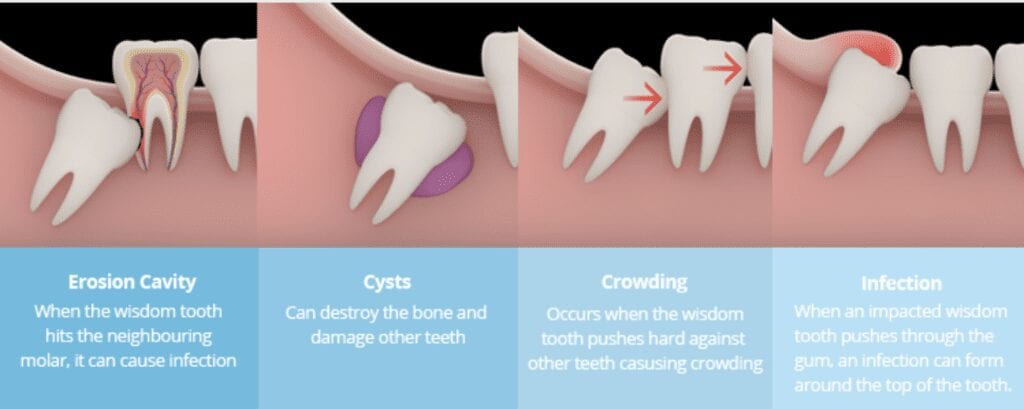
Gum Disease – When a wisdom tooth partially breaks through the gum’s surface, bacteria can get under the flap, causing an infection in the gum.
Crowding – An impacted or erupting wisdom tooth can push on adjacent teeth, causing them to become crooked or even damaging them structurally.
Decay – A wisdom tooth that is hard to clean due to its position or because it is partially covered by gum tissue may collect cavity-causing bacteria. This could also lead to decay in the tooth next to it.
Poor Position – A wisdom tooth that grows toward the cheek can irritate nearby tissue. If an erupted tooth is crooked, it may be hard to clean and can even make it hard to bite down.
Cysts – If the sac that holds the crown remains in the bone, it can fill with fluid, forming a cyst that can destroy surrounding bone.
Types of Impactations
Your Dental and Medical History
Your dentist may ask whether you have tooth or jaw pain or sensitivity to cold or hot foods, about prior dental treatment and about gum or jaw problems. You may be asked about medical problems that could interfere with treatment. Be sure to tell your dentist about medications you’re taking because they could affect treatment.
Your Dental Examination
An examination helps us determine the general heath of your mouth as well as that of your wisdom teeth. We may inspect your gums and jaws for swelling, tenderness or infection. Your teeth may be examined for the presence of tooth decay. Your blood pressure, pulse and respiration may be checked to assess whether you can undergo anesthesia.
Taking Dental X-rays
To help confirm the diagnosis, we will take x-rays. X-rays are especially useful for identifying potential problems when you don’t have symptoms. Intraoral x-rays are small and provide an internal view of the individual teeth and jawbone. If intraoral x-rays don’t provide enough information, other types of x-rays may be needed such as panoramic x-rays. They provide a clear image of the area around all four wisdom teeth as well as surrounding bone. These x-rays can show hard-to-image impacted teeth clearly.
Risks and Complications
If you decide on removal, we will discuss the risks and possible complications with you and ask you to sign a consent form. Removal of wisdom teeth is a common procedure but as with any surgery, there are risks such as side effects from the anesthetic, bleeding or infection and possible complications such as numbness.
Numbness – Impacted teeth may be close to or in actual contact with the nerves that supply sensation to the teeth, gums, tongue, chin, cheeks and lips. Occasionally these nerves are injured when the tooth is removed, causing numbness and tingling. If this happens, the nerve usually repairs and regenerates itself within a short time. In some cases, numbness is permanent.
Dry Socket – Healing can be delayed if the blood clot covering the socket dissolves or is washed away. This exposes the bone and may lead to constant, deep, throbbing pain, which can easily be treated with a dressing.
Infection – Infection is a less common complication. It can usually be treated by draining the infection or with antibiotics.
Sinus Problems – Because the upper wisdom teeth are near a sinus cavity, the removal of these teeth can open the sinus cavity on rare occasions. The sinus usually heals, but if a problem persists, further treatment may be needed.
Weakening of the Jaw – In rare cases, removal of an impacted tooth can weaken the jaw, making it more susceptible to fracture.
Your Surgery Experience
You may need to take some days off work or school to give yourself enough time to recover. Schedule enough time to recover. Schedule a follow-up visit with us so we can monitor your progress after surgery and check that you’re healing properly.
Eating – If your surgery is going to include anesthesia or intravenous (IV) medication, don’t eat or drink anything after midnight the night before. Otherwise, don’t eat or drink anything for at least six hours before surgery.
Transportation – You’ll probably be tired and not alert enough to drive home safely after surgery. Arrange to have a responsible adult come with you on the day of surgery who can drive you home.
Clothing – Wear loose, comfortable clothes. Choose a shirt or blouse with short sleeves so if you receive an IV (intravenous) anesthetic, it can be administered easily.
Before Surgery – A local anesthetic is used to numb the area around each wisdom tooth being removed.
During Surgery – Expect the procedure to take about an hour. If your tooth is erupted, it may be removed (extracted) from its socket without an incision in your gum. For impacted teeth, an incision will be necessary. Stitches may be use to close the incision.
After Surgery
You’ll rest for a while under close observation as you recover from the anesthetic. When your dentist or oral surgeon is satisfied with your progress, you’ll be able to go home. You may get a prescription for pain medication as well as instructions for your home recovery. Plan to rest at home for the remainder of the day. During the next few days, don’t plan on driving, drinking alcohol or operating any kind of machinery; you may be drowsy from the pain medication, other drugs or anesthetic.
The Healing Process
The healing process begins immediately after surgery. The body sends blood to nourish the tooth socket. To control excessive bleeding, you may be instructed to bite down on a piece of gauze, applying constant, direct pressure to the area. This helps a blood clot to form in the socket. In a day or two after surgery, soft tissue begins to fill in the opening. New bone tissue also begins to grow in the socket, becoming denser over the next two to three months.
Pain and Swelling
As the anesthetic or pain medication that you received at the facility wears off, you may experience some discomfort. Your gums and jaw may feel tender and sore. To make yourself more comfortable, take the pain medication that has been prescribed. It’s normal for your cheek to swell, but you can keep swelling to a minimum by placing ice packs on your cheeks during the first 24 hours after surgery.
Healing Tips
- DO apply pressure to stop the bleeding by placing the gauze directly over the extraction site.
- DO eat soft foods, such as soups and blenderized meals after the bleeding stops.
- DO drink lots of fluid after the bleeding stops.
- DO take antibiotics or pain-reducing medication if prescribed.
- DO keep your mouth clean.
- DON’T chew hard or crunchy foods such as carrots or popcorn for 2 weeks. These foods could become lodged in the extraction site or fracture the weakened jawbone.
- DON’T brush the teeth in the area of surgery until the day after surgery. Brush carefully.
- DON’T rinse your mouth or spit forcefully the day of surgery; it could loosen the blood clot.
- DON’T smoke after surgery. Inhaling creates suction and it could loosen the blood clot.
- DON’T over exert yourself.
- DON’T use alcohol the day of surgery or while taking pain medications.
ORAL SURGERY & WISDOM TOOTH EXTRACTION
|
|
THB |
Duration |
|
Normal Tooth Extraction |
1,500–2,500 |
1 Visit |
|
Complicated Tooth Extraction |
2,500–3,500 |
1 Visit |
|
Wisdom Tooth Extraction (Fully erupted) |
4,000 |
1 Visit |
|
Wisdom Tooth Extraction (Partially impacted) |
5,000–9,000 |
1 Visit |
|
Wisdom Tooth Extraction (Fully embedded) |
10,000–15,000 |
1 Visit |