Root Canal Treatment In Bangkok, Thailand
ROOT CANAL TREATMENT (ENDODONTICS)
Natural teeth are meant to last a lifetime. Even if one of your teeth should become critically injured or diseased, it can oftentimes be saved through a specialized dental procedure know as endodontic (Root Canal) treatment commonly called a root canal. Although this technique has been around for several decades, recent advances in the field of endodontics have made root canal therapy almost a routine procedure.
To help you understand when and why such a procedure might be needed and how a damaged tooth can be saved, we have answered some of the most frequently asked questions about endodontic treatment.
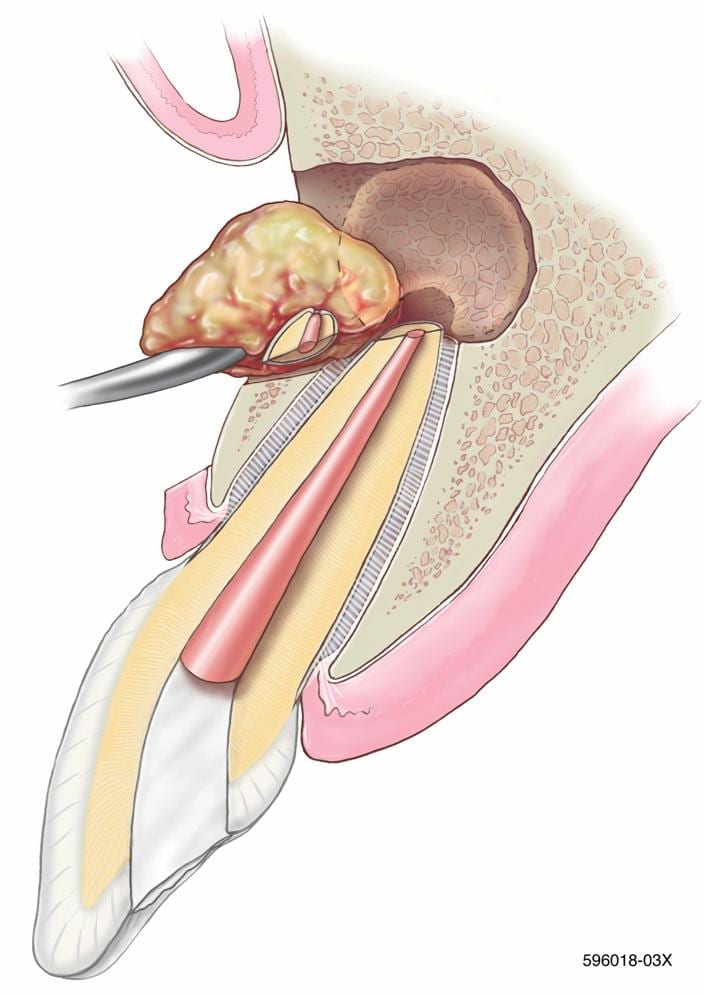
What is endodontic treatment?
Endodontics is the area of dentistry concerned with the prevention, diagnosis and treatment of disorders of the dental pulp (the tooth’s soft core). Years ago, teeth with diseased or injured pulps were extracted. Today, endodontic treatment gives dentists a safe and effective means of saving teeth.
What is the dental pulp?
The pulp is a soft tissue that contains the nerves, arteries, veins and lymph vessels of a tooth. It lies within the dentin, the bone-like tissue that supports the enamel. Within the dentin, the pulp extends from the pulp chamber in the crown (the portion of the tooth visible above the gums) down to the tip of the root by way of the root canal. All teeth have only one pulp chamber, but teeth with more than one root with have more than one canal.
What happens to the damaged pulp?
When the pulp is diseased or injured and unable to repair itself, the pulp dies. The most common cause of pulp death is a fracture or a deep cavity that exposes the pulp to saliva. The bacteria found in saliva causes infection inside the tooth. Left untreated, the infection eventually causes the pulp to die. Pus builds up at the root tip, forming an abscess that can destroy the supporting bone that surrounds the tooth.
Why does the pulp need to be removed?
If the damaged or diseased pulp is not removed, the tooth and surrounding tissues become infected. Pain and swelling may accompany the infection. Even in the absence of pain, certain by-products of a diseased pulp can injure the bone that anchors your tooth in the jaw. Without endodontic treatment, your tooth will eventually have to be removed.
What does endodontic treatment involve?
Treatment usually requires from one to three appointments. During these treatments, your dentist or endodontist (a dentist who specializes in disorders of the pulp) removes the diseased pulp. The pulp chamber and root canal(s) of the tooth is then cleaned, shaped, filled and sealed to prevent recontamination of the root canal system.
Here is how your tooth is saved through endodontic treatment:
- First, the tooth is isolated from the saliva with a rubber dam (a sheet of rubber placed around the tooth). An opening is then made through the crown of the tooth into the pulp chamber. You may be given a local anesthetic prior to this step so that you will be more comfortable during treatment.
- The pulp is then carefully removed from both the pulp chamber and root canal(s). The root canal(s) is cleaned, enlarged and shaped to a form that can be properly filled.
- Medication may be put in the pulp chamber and root canal(s) between appointments to help eliminate bacteria and prevent infection.
- A temporary filling will be placed in an opening in the crown of the tooth to protect the pulp chamber and root canal(s). If the pulp was severely infected, your dentist may leave the tooth open for a few days to drain. You may also be given antibiotics to help the body control infection that has spread beyond the tooth.
- During the next stage of treatment, the temporary filling is removed. The pulp chamber and root canal(s) are then filled and permanently sealed with a material that prevents bacteria from re-entering the canal.
- In the final step, a gold or porcelain crown is usually placed over the tooth to restore the tooth’s structure, function and appearance. If an endodontist performs the treatment, he or she will recommend that you return to your family dentist for this final step.
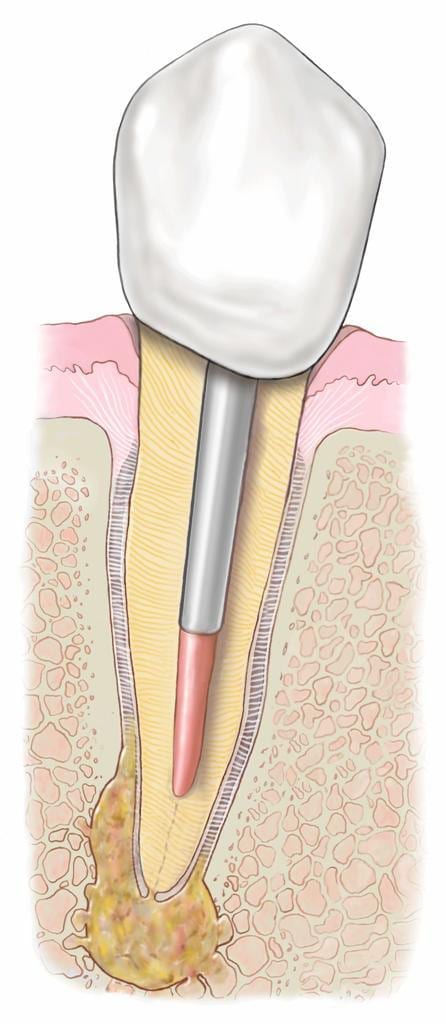
The type of material used for the crown will depend on where the tooth is located in your mouth, the color of the tooth and the amount of natural tooth remaining. A front tooth that affects appearance, for instance, most likely will be restored with a porcelain or a porcelain-fused-to-metal crown. When a back tooth has been badly fractured or decayed, a gold or porcelain-fused-to-metal crown may be used. Your dentist will discuss these options with you.
Why couldn’t you just remove the tooth?
The choice is yours but there are many disadvantages to losing a tooth. When a tooth is removed and no replaced, the teeth next to the empty space begins to shift from their normal position. This may cause teeth to become crooked or crowded, which then decreases chewing and biting efficiency. Crowded or crooked teeth may be more prone to dental disease because they are harder to keep clean than properly aligned teeth. As a result, other teeth may be lost if the missing tooth is not replaced.
A replacement tooth (an implant or a bridge) is usually more expensive than endodontic treatment and involves more extensive dental procedures on adjacent teeth. Endodontic treatment can safely and comfortably save a tooth that otherwise would have to be removed. In fact, root canal therapy is successful approximately 95% of the time. Remember, a healthy restored tooth is always better than an artificial one.
How long will the restored tooth last?
Your endodontically treated and restored tooth could last a lifetime, if you continue to care for your teeth and gums. As long as the root(s) of an endodontically treated tooth are properly nourished by the surrounding tissues, you tooth will remain healthy.
ENDODONTICS (ROOT CANAL TREATMENT)
|
THB |
Duration |
|
|
Anterior/Incisor Tooth (Front tooth) |
THB 11,000 per tooth USD 340 GBP 249 AUD 519 NZD 561 |
1-2 Visits |
|
Premolar Tooth |
THB 14,000 per tooth USD 433 GBP 317 AUD 660 NZD 714 |
1-2 Visits |
|
Molar Tooth |
THB 17,000 per tooth USD 526 GBP 385 AUD 802 NZD 867 |
1-2 Visits |
|
Retreat Root Canal |
add THB 2,000 per tooth USD 62 GBP 46 AUD 95 NZD 102 |
|
|
Root Filling |
THB 2,000 per tooth USD 62 GBP 46 AUD 95 NZD 102 |