Even though the most requested cosmetic dental procedure available in the United States of America is tooth or teeth whitening, it takes more than bleach to end up with a smile of perfect pearly whites. You need to be quite hygienic with your mouth to maintain dental healthiness. When it comes to dental extraction, it’s probably one of the most requested dental procedures as well. To wit:
• Everyone has probably suffered from cavities or dental caries sometime in their lifetimes.
• According to the NIDCR, 92 percent of American adults from 20 to 64 years of age have suffered from at least one cavity in their permanent teeth.
• Not to mention the child’s tendency to get cavities in their milk teeth (but the consequences for that isn’t so dire since primary teeth tend to fall out anyway).
Procedure

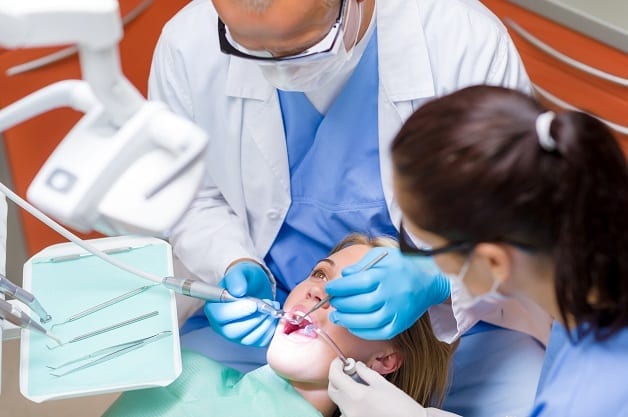
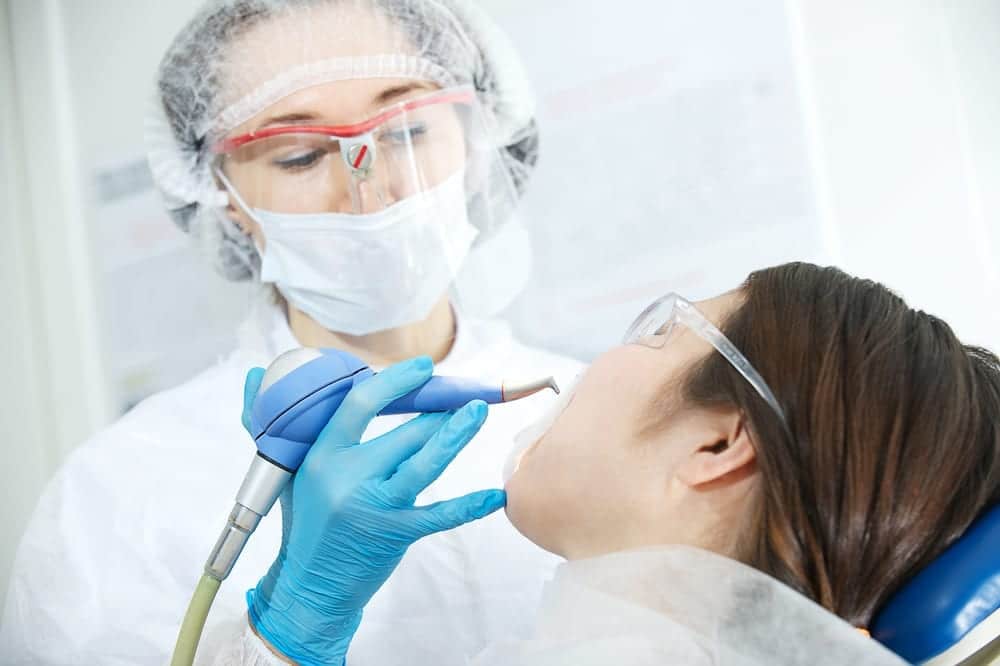
Here’s the deal when it comes to doing a simple dental extraction. Pulling teeth is typically managed by your dentist alone and it’s a relatively simple procedure. This is what you should expect.
1. Anesthesia: Local anesthesia is used to numb your teeth and gum area prior to pulling. This type of anesthesia only numbs down a local area of your body (as opposed to general anesthesia, which involves putting you to sleep during a treatment or surgery).
2. Tools for Extraction: The tools used for tooth extraction involve a pair of forceps and an elevator.
a. Elevator: In the context of dentistry, an elevator refers to a tool used to separate the tooth root from the tooth socket, loosening it from the bone altogether.
b. Forceps: Meanwhile, the forceps loosen the tooth out. It’s the tool that yanks the loosened tooth from its crown.
3. Stitches: Sometimes, depending on the size of the tooth (maybe it’s a molar, canine, or incisor), stitches might be required to close up the extraction site. Maybe it took more force from the forceps and elevator to get the tooth, leading to a larger, deeper wound then intended. Usually, it’s not called for.
As for the surgical extraction of the tooth, it’s a little more complicated and involves more cutting and stitches. It’s also typically done in order to fix wisdom tooth impactions and other complex dental maladies. It involves the following:
1. Removal of Tooth from Bone: Surgical dental extraction is different from simple dental extraction, mainly because the former involves removal of the tooth from the bone.
2. Surgery Done by Surgeons: An ordinary dentist is not enough to perform the surgical tooth extraction, which is mainly a form of dental surgery (as the name suggests). It requires the help of maxillofacial and oral surgeons.
3. More Anesthesia Options: Depending on the complexity or severity of the tooth extraction, you might be given local or general anesthesia. In other words, they can numb the area or put you to sleep to perform the surgical procedure.
4. Gum Cutting and Stitching Back: With simple extraction, forceps and an elevator is enough to extract the tooth by its crown. With surgical extraction, the gum is cut open to access the tooth or teeth, especially when it comes to wisdom teeth impactions.
5. Drills, Cuts, Fillings, and Stitches: The surgeon is typically tasked to remove teeth (as a whole or in fragments) from within the jaw bone. Afterwards, stitches are required to close the wound.
Pain and Complications to Watch Out For

After the tooth has been pulled from simple extraction, you will typically be asked by your dentist to bite down on a pack of gauze or cotton. This pressurized biting will help speed up blood clot formation within the socket. This will lead to uneventful and healthy healing. As the liberal use of anesthesia for this procedure suggests, though, teeth extractions of permanent teeth can get quite painful (especially once the anesthesia wears off).
Nevertheless, watch out for the following tooth pain issues and complications that could lead to further suffering down the line.
• Swelling and Pain: There should be some pain and swelling after the operation. That’s normal. The level of pain worsens the more teeth is extracted from your mouth. The pain can also go from mild to severe to the type of extraction method (simple to surgical tooth extraction), the location of the extraction, and if there’s any coexisting infection available. Your personal pain tolerance can also serve as a factor of sorts. If the pain persists and worsens after two or more days, you might have an infection or a dry socket syndrome.
The pulp is the organic part of the tooth from within its enamel and dentin shell that contains the blood vessels and nerves keeping it alive and allowing it to gauge hot and cold sensations. This is where bacteria can form, leading to antibiotic therapy, root canal therapy, or dental extraction that keeps the infection from spreading. Infection can also happen after the tooth is extracted, which has to be dealt with before other teeth are affected.
• Risk of Infection and Dry Socket: The socket area where your tooth was extracted could totally swell and end up infected after the operation. This entails antibiotics, ice packs to keep the swelling down, and the dentist draining fluid from the site of the swelling. If your immune system is compromised from organ transplant or chemotherapy, your risk of infection could rise as well.
Another complication you want to avoid when it comes to post-operation dental extraction is a dry socket syndrome. Although this is rare and affects 2 percent of extraction patients, it does happen. It typically involves having whitish bone instead of a blood clot over the extraction site and severe pain two days after the operation. It also leaves a bad taste and smell in your mouth.
• Periodontal Disease: Be wary of infection risks and leftover bacteria from your diseased tooth that could lead to gingivitis and periodontitis down the line. Both diseases can induce extraction and serve as complications post-operation, resulting in a negative feedback loop that destroys all your teeth.
This infection of the bones and tissues surrounding and supporting teeth can loosen teeth if not dealt with post-haste. It should be treated during the gingivitis phase before it turns into full-blown periodontitis that requires expensive teeth scaling and deep cleaning on top of tooth extraction.
Healing Time
It takes longer for you to heal if stitches were involved or the clot is dislodged. However, it’s also normal to feel mild to moderate pain as well as swelling as the socket heals. Just remember that if these symptoms persist, consult your dental professional. He’ll know what to do.
With that said, here are the stages of healing for a dental or tooth extraction.
• Blood Clot Formation: There should be a blood clot forming in the empty socket where your tooth was once attached to. Without it, you could end up developing dry socket or an infection in the area.
• Things to Avoid: In order to facilitate healing, you should avoid sucking, spitting, and rinsing until the area has healed up. Also, avoid smoking after a tooth extraction since that could disrupt blood clot formation dislodge the clot from the socket.
• When Will the Pain Subside? After getting your tooth extracted during the first 24 hours, expect bleeding to continue throughout the day or at least a few hours after extraction took place. It typically takes about a day or two for the wound to stop bleeding and start healing. Your gum pain should subside around this time as well.
• When Will the Socket Wound Close? It takes one to two weeks for the dental extraction site or damaged tooth socket to heal up (if there are no complications involved), forming a layer of gum over where your tooth used to be. Meanwhile, it takes about a month for both bone and soft tissues to continue healing themselves.
• Damaged or Dislodged Clot: If your clot becomes dislodged or damaged, this could lead to the bone or nerve underneath your gums to get exposed to outside elements such as debris, saliva, air, and food. This exposure should then lead to an infection or a dry socket syndrome.
• Dry Socket Treatment: If you do end up with dry socket, consult your dentist on what to do. You will probably have to undergo extensive wound cleaning and a cocktail of antibiotics to encourage your gums to make that healing blood clot. Thankfully, only 2 to 5 percent of patients end up with this malady.
Aftercare

In regards to aftercare for your dental extraction operation, here’s what you should keep in mind. It only takes a few days to recover as mentioned above, but you should observe proper aftercare procedures to ensure that everything comes off without a hitch. You shouldn’t rest too easy, even after the swelling and bleeding has ended.
It takes weeks and upwards to a month to fully heal from a dental extraction. You should be careful and do what’s required of you in the first 24 hours after the procedure. Have the presence of mind to do the following until the socket area is fully healed or until the stitches come out. To wit:
• In the first 24 hours, don’t favor the wound or keep touching it with your tongue so that it won’t end up traumatized or prolong its healing process. Leave it alone!
• Another way to promote healing or improve the extraction healing timeline is to keep the extraction site as clean as possible.
• Chew your food away from the site where your tooth was extracted.
• The socket might require irrigation from your dentist, but it’s his call whether it’s needed or not. Usually, you don’t have to go through this.
• Once you’ve survived through the worst of the pain, your stitches might be altogether removed if stitches were involved in closing up your extraction wound.
In regards to the management of post-extraction complications, you should do the following.
• Consult your dentist right away if you’re suffering from:
o Muscle or joint pain
o Tooth chips or bone fragments
o Dry sockets
o Continued or persistent pain
o Bruising
o Swelling
o Prolonged building
• Your dentist will know what to do in regards to treating those individual symptoms one-by-one or all at the same time depending on how many dental extraction complications you’re suffering from.
• The dental professional might irrigate the area, drain it of fluid if it’s swelling, apply antibiotics to fight off the infection, or a host of other potential treatments to jumpstart the healing process.
• Your treatment options will depend on your unique circumstances and biology, so inform your dentist of everything he needs to know about you (like preexisting conditions or any medications you’re currently taking) so that he can tailor the right solution for your dental extraction dilemmas.
• Usually, aftercare treatment at the dental clinic is free of charge and is an extension of the tooth extraction procedure you’ve already paid for. Talk to your dentist if that’s the case or not.
• Naturally, if you’re dealing with aftercare for impacted wisdom tooth extraction, the healing process will take longer than a simple, non-surgical removal of a diseased tooth due to all the drilling, gum cutting, and bone penetration involved to access the wisdom tooth in the first place.
Why Do People Have Their Teeth Pulled?
People tend to fix such holes in their teeth with dental filling, but when bad comes to worse and even a root canal (endodontic) therapy isn’t enough to fix your damaged, infected tooth with a throbbing tooth root, a tooth extraction is definitely called for. This is why you shouldn’t leave dental caries untreated and you should always observe proper dental hygiene every time.
A dental extraction is usually done when you cannot afford root canal therapy and you’ve decided that the painful tooth is disposable and can be replaced in the future with a denture, bridge, or dental implant. This severe happens whenever the damage extends all the way to the tooth root and pulp or the center of the tooth itself.
Thantakit International Dental Center is Thailand’s longest established dental center. Situated in Bangkok, our clinic is renowned across the world as a destination for world-class dentistry, with most of our patients flying to us from Australia.
Please contact us today and get a FREE dental consultation